New
» Go to news mainUpdates to Reporting Computed Tomography Angiograms of Acute Aortic Syndromes
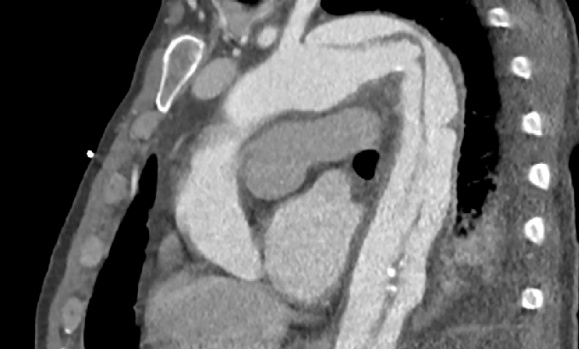
See update from Dr. Andreu Costa and Dr. Bruce Precious
Summary
In their review article, Modares et al.1 have provided a comprehensive and beautifully illustrated overview of acute aortic syndromes. Although the 3 main acute aortic pathologies are well known to radiologists, Modares et al. provide us with up-to-date entities perhaps less familiar to radiologists, such as intramural blood pool, ulcer-like projections and limited intimal tear.1,2 The authors also highlight imaging pitfalls and considerations for reporting CT examinations of these entities, in light of management and follow-up.
In 2020, the Society for Vascular Surgery and Society of Thoracic Surgeons (SVS-STS) published a consensus on standards for reporting type B dissections.3 Research over the last several years has led to an improved understanding of the pathophysiology, natural history and management of aortic dissections, particularly with the use of thoracic endovascular aortic repair.4 With ongoing scientific advances, the treatment of type B dissections is evolving rapidly, and may include medical, surgical and endovascular options provided by a variety of specialists, including vascular surgeons, cardiothoracic surgeons, cardiologists and interventional radiologists.3 Hence, the need for an up-to-date, comprehensive standard to classify acute aortic syndromes. The SVS-STS reporting standards provide a “unified consensus on reporting, nomenclature and classification of type B aortic dissection.”3 These standards overcome several deficiencies of the Debakey and more simplified Stanford classifications systems, which date back to 1965 and 1970, respectively. The limitations of these older systems include: 1) inconsistent classification of dissections arising from the aortic arch (both systems); 2) lack of distant extent description (Stanford); 3) exclusion of aortic syndromes other than dissection (DeBakey); and 4) unclear nomenclature for dissections with proximal extent.1,3,4
The SVS-STS reporting standards classify aortic syndromes according to the site of the entry tear: type A dissections have entry tears arising from zone 0, which corresponds to the ascending aorta including the ostium of the brachiocephalic artery; and type B dissections have entry tears arising distal to the brachiocephalic artery, including those with retrograde extension to the ascending aorta. An indeterminate type I is used to classify dissections that involve the ascending aorta and extend distal to the brachiocephalic artery, but cannot be classified as A or B because the entry tear is not evident. A type A dissection extending to zone 4 would be labeled A4, and a type B dissection arising from zone 2 and extending to zone 9 (corresponding to the infrarenal aorta) would be labeled B2,9. The subscripts denote the extent of involved aorta and include both patent and thrombosed false lumen, as well as intramural hematoma.3
Should radiologists adopt the SVS-STS standard when reporting CTA examinations of acute aortic syndromes? According to the Writing Committee of the SVS-STS guidelines, “it is not necessarily the intent […] that the new classification system should completely replace the current Stanford and DeBakey systems for everyday clinical use, especially for practitioners who are not subject matter experts in aortic disease.”3 Modares et al. agree, stating that the 2020 SVS-STS standards “may not be relevant for physicians who are not experts in the diagnosis and management of aortic diseases.”1 Indeed, the SVS-STS guidelines provide a comprehensive, precise classification scheme that can be used for research studies evaluating the management and outcomes of acute aortic syndromes.
In our opinion, the SVS-STS standards provide a straightforward nomenclature to succinctly describe acute aortic syndromes. Nevertheless, for the radiologist reporting CTAs of acute aortic syndromes, it is worth noting that the single most important factor that determines management of an acute aortic syndrome is whether the ascending aorta is involved (type A) or not (type B). This distinction is what impacts immediate management decisions in the hyperacute setting (defined by the SVS-STS standards as less than 24 hours).
Irrespective of the nomenclature used, there are a number of elements to include in CTA reports of acute aortic syndromes, and several of these are provided by Modares et al.1 For example, high-risk features of a type B dissection include an entry tear larger than 1 cm or along the inner curve of the arch, an aortic diameter larger than 4 cm at presentation, and a partially (not completely) thrombosed false lumen.1 Other radiographic features defined as high-risk by the SVS-STS standards are a bloody pleural effusion, a false lumen diameter over 2.2 cm, and imaging evidence of malperfusion.3
In summary, as the management of acute aortic syndromes continues to evolve, the SVS-STS standards provide an up-to-date, consensus-based classification scheme that overcome limitations of the DeBakey and Stanford systems. A potential avenue for the radiology community to consider, as we gain clarity on the specific imaging features that impact treatment decision-making and prognosis, is to create a standardized synoptic reporting template or algorithm, as suggested by some groups,2 to provide high-quality, accurate and comprehensive CTA reports.
Recent News
- Dr. Abraham receives CAIR Award
- Thank you to everyone who joined us for the 30th anniversary Radiology Research Day on May 8th!
- Nova Scotia’s Lung Screening Program expanding to Cape Breton, eastern mainland
- Donor‑supported nuclear medicine technology attracts top medical talent to the QEII
- Building Critical Skills at the Dalhousie Physician Leadership Workshop for Women in Radiology
- CAR/CSTR Practice Guideline on CT Screening for Lung Cancer
- CAR/CSACI Practice Guidance for Contrast Media Hypersensitivity
- CAR Practice Guideline on Bone Mineral Densitometry Reporting: 2024 Update
